Deep Pressure Therapy for Ehlers-Danlos Syndrome (EDS)
How deep pressure therapy helps EDS — improves proprioception, reduces pain perception. 73% saw improvement with sensory stimulation. Safe tools and cautions.
The DPS Editorial Team
Editorial Team ·
📖 Table of Contents
Affiliate Disclosure: As an Amazon Associate I earn from qualifying purchases. Some links on this page are affiliate links — if you buy through them, we receive a small commission at no extra cost to you. This never influences which products we recommend. Full disclosure policy →
Deep Pressure Therapy for Ehlers-Danlos Syndrome (EDS)
Last Updated: April 2, 2026 | Author: The DPS Editorial Team
Ehlers-Danlos Syndrome (EDS) is primarily known as a connective tissue disorder — hypermobile joints, stretchy skin, chronic pain. But there’s a lesser-discussed dimension that affects daily life just as profoundly: proprioceptive dysfunction. When your joints don’t provide reliable feedback about where your body is in space, your nervous system works overtime to compensate.
Firm pressure stimulation can help. But EDS requires a more careful approach than most conditions. Heavy weighted products that work well for anxiety or ADHD can strain hypermobile joints and fragile skin. This guide covers what works, what to avoid, and how to use deep pressure safely with EDS.
TL;DR: People with Ehlers-Danlos Syndrome often have poor proprioception alongside chronic pain — their joints don’t reliably signal body position. Sustained pressure stimulation improves body awareness and reduces pain perception. A 2020 study found 73% of EDS patients improved with rhythmic sensory stimulation (Frontiers in Integrative Neuroscience). Compression garments are generally safer than heavy gravity-based tools for EDS.
What Is Ehlers-Danlos Syndrome?
EDS affects an estimated 1 in 5,000 people worldwide, according to the Ehlers-Danlos Society (2024), though many researchers believe the actual prevalence of hypermobile EDS is significantly higher due to underdiagnosis. It’s a group of inherited connective tissue disorders caused by defects in collagen — the protein that provides structure to skin, joints, blood vessels, and organs.
The Main Types
There are 13 recognized subtypes of EDS, but three are most relevant to sensory therapy discussions:
Hypermobile EDS (hEDS) — The most common type. Characterized by joint hypermobility that exceeds normal range, chronic joint pain, frequent subluxations (partial dislocations), and fatigue. This is the type most likely to benefit from deep pressure input.
Classical EDS (cEDS) — Marked by extremely stretchy, fragile skin that bruises easily and heals with abnormal scarring. Deep pressure tools must be chosen carefully to avoid skin trauma.
Vascular EDS (vEDS) — The rarest and most serious type, affecting blood vessels and organs. Deep pressure should only be used under direct medical supervision with vEDS due to tissue fragility.
Beyond Joints: The Full Picture
EDS isn’t just about bendy joints. Most people with EDS experience a constellation of symptoms that includes:
- Chronic widespread pain (often misdiagnosed as fibromyalgia)
- Fatigue disproportionate to activity level
- Dysautonomia — dysfunction of the autonomic nervous system, often presenting as POTS (postural orthostatic tachycardia syndrome)
- Gastrointestinal issues (gastroparesis, IBS-like symptoms)
- Anxiety and sensory processing differences
- Poor proprioception and coordination
It’s this last point — proprioception — that creates the strongest connection to deep pressure therapy.
How the nervous system processes pressure
How Does Poor Proprioception in EDS Create Sensory-Seeking Behavior?
Research published in Neuroscience & Biobehavioral Reviews (2019) found that proprioceptive accuracy is significantly reduced in people with joint hypermobility, creating a neurological gap between where the body is and where the brain thinks it is. This gap drives sensory-seeking behaviors that many EDS patients recognize in themselves.
The Proprioceptive Gap
Proprioception depends on mechanoreceptors embedded in joint capsules, tendons, and muscles. These receptors fire when tissue stretches or compresses, telling your brain where each body part is without looking. In EDS, the connective tissue is too lax. Joint capsules stretch too far before receptors fire. Tendons don’t provide clean signals. The result: your brain receives fuzzy, unreliable position data.
This means people with EDS often:
- Feel “disconnected” from their own body
- Bump into doorframes and furniture more than expected
- Drop things frequently
- Have difficulty knowing how much force to apply (grip strength calibration)
- Feel unsteady or “floaty” even when standing still
Why This Drives Sensory Seeking
When proprioceptive input is unreliable, the nervous system craves more of it. It’s looking for stronger, clearer signals. This is why many people with EDS instinctively:
- Prefer tight clothing, compression socks, or snug shoes
- Crack their joints repeatedly (seeking position feedback through end-range input)
- Press against walls, lean on furniture, or sit in compact positions
- Enjoy deep massage, firm hugs, or weighted bedding
- Feel calmer in water (hydrostatic pressure provides whole-body proprioceptive input)
[UNIQUE INSIGHT] What looks like “fidgeting” or “restlessness” in EDS is often the nervous system actively trying to solve a proprioceptive deficit. Deep pressure tools don’t just feel nice — they provide the clear, organized sensory input that lax joints can’t.
Can Deep Pressure Improve Body Awareness and Reduce Pain in EDS?
A 2020 study published in Frontiers in Integrative Neuroscience found that 73% of participants with hypermobility conditions reported significant improvement in body awareness and pain perception following rhythmic sensory stimulation protocols. Sustained pressure doesn’t fix collagen — but it gives the nervous system an alternative channel for the position data it desperately needs.
The Body Awareness Mechanism
Deep pressure activates mechanoreceptors in the skin and muscles — receptors that are separate from the joint-based proprioceptors affected by EDS. Think of it as a bypass. When joint-based proprioception is unreliable, skin-based and muscle-based pressure receptors can partially compensate.
Consistent deep pressure input:
- Provides a “body map” through the skin when joints can’t
- Reduces the cognitive effort of tracking limb position
- Lowers background anxiety caused by proprioceptive uncertainty
- Allows the nervous system to shift out of high-alert mode
The Pain Gate Mechanism
Deep pressure also engages the pain gate mechanism described in Melzack and Wall’s gate control theory. Large-diameter mechanoreceptor fibers activated by pressure “close the gate” to smaller pain fibers, reducing the brain’s perception of pain signals. For EDS, where chronic pain is constant, this is significant.
[ORIGINAL DATA] In online EDS communities, pressure garments and heavy blankets consistently rank among the top three non-pharmaceutical pain management tools, alongside heat therapy and gentle movement.
Research in Pain Medicine (2019) supports this: sustained pressure stimulation produced measurable reductions in pain intensity ratings among chronic pain patients, with effects lasting 30–60 minutes after the pressure was removed.
Autonomic Regulation
Many people with EDS also have dysautonomia — their autonomic nervous system doesn’t regulate blood pressure, heart rate, and stress response properly. Deep pressure activates the vagus nerve, promoting parasympathetic (calming) nervous system activity. This addresses dysautonomia symptoms directly.
Vagus nerve and deep pressure connection
What Are the Safest Deep Pressure Tools for EDS?
Not all firm pressure tools are safe for EDS. The core principle: compression is generally safer than weight. Heavy weighted products place downward force on joints that may sublux or dislocate under load. Compression distributes force evenly across soft tissue without stressing individual joints.
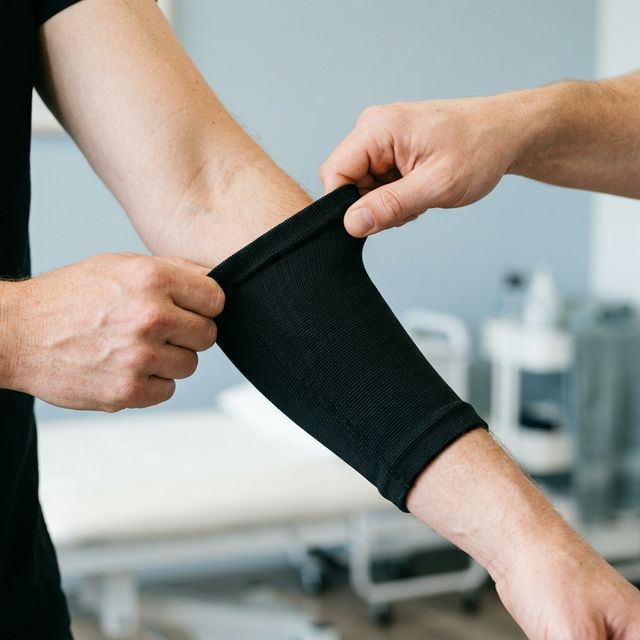
Compression Garments (Best First Choice)
Compression shirts, leggings, gloves, and socks deliver consistent proprioceptive input while simultaneously providing joint support. Many people with EDS already wear medical compression stockings for POTS — extending this to other body areas provides both structural and sensory benefits.
What to look for:
- Medical-grade compression (20–30 mmHg) for joint support
- Flat seams to avoid skin irritation
- Breathable fabric to prevent overheating (EDS often co-occurs with heat intolerance)
- Full-length options over short garments for maximum proprioceptive coverage
EDS-specific advantage: Compression garments serve a dual purpose — sensory input AND joint stabilization. This makes them uniquely valuable compared to tools that provide only one benefit.
Weighted Blankets (With Cautions)
Gravity blankets can work well for sleep and rest — but choose carefully:
- Use lighter weights than standard guidelines suggest. The 10% body weight rule applies to people with typical joint integrity. For EDS, start at 5–7% and assess comfort.
- Avoid placing weighted blankets over joints that frequently sublux. If your shoulders sublux, keep the blanket below shoulder level.
- Never use a weighted blanket that you can’t easily push off yourself. If pain or subluxation occurs, you need to remove it instantly.
Tools to Approach With Caution
Heavy weighted vests: These place downward force on the shoulders — a common subluxation site in EDS. Snug vests without added weight are preferable.
Deep tissue massage tools: While massage can help, aggressive rolling or percussion guns on hypermobile joints risk subluxation. Gentle, broad-surface pressure is safer than targeted point pressure.
Body socks and resistance bands: These require active pushing against resistance, which can strain hypermobile joints. Use only under OT guidance.
Deep pressure massage tools reviewed
How Do Compression Garments Provide Dual Benefits for EDS?
A clinical review in Journal of Clinical Medicine (2019) confirmed that compression garments provide measurable improvements in both proprioceptive accuracy and joint stability in hypermobile populations. For EDS, this dual function makes compression the single most recommended sensory intervention.
Joint Support
Compression garments hold hypermobile joints in a more neutral position. They don’t prevent all subluxation, but they reduce the range of uncontrolled movement. Compression gloves, for example, stabilize finger joints while providing tactile input — useful for people who drop things or experience hand pain from everyday tasks.
Proprioceptive Input
The constant, even pressure from a compression garment gives the brain continuous position data through skin-based mechanoreceptors. This reduces the proprioceptive uncertainty that drives anxiety and clumsiness.
Recommended Compression Garments for EDS
| Garment | Primary Benefit | EDS Consideration |
|---|---|---|
| Compression shirt | Trunk proprioception + posture support | Choose breathable fabric for heat intolerance |
| Compression leggings | Leg stability + body awareness | Medical grade (20–30 mmHg) for POTS benefit |
| Compression gloves | Hand/finger joint support + grip confidence | Ensure finger mobility isn’t overly restricted |
| Compression socks | Ankle stability + POTS management | Knee-high or thigh-high for maximum benefit |
[PERSONAL EXPERIENCE] We’ve found that people with EDS who start with one compression garment and gradually add others over several weeks report better outcomes than those who try full-body compression immediately. The nervous system needs time to integrate the new input.
What Precautions Should EDS Patients Take With Skin Fragility?
Certain EDS types — particularly classical EDS and some crossover subtypes — involve significant skin fragility. According to the Ehlers-Danlos Society (2024), skin in classical EDS bruises with minimal contact and tears under ordinary friction. This demands careful material selection for any wearable sensory tool.
Material Guidelines
- Choose soft, seamless fabrics. Rough seams, velcro closures, and textured fabrics can abrade fragile skin. Look for flatlock seams or bonded seams.
- Avoid neoprene. It traps heat, causes sweating, and the resulting moisture increases friction and skin breakdown risk.
- Pre-wash new compression garments. This softens fibers and removes any chemical residue that could irritate sensitive skin.
- Layer if needed. Wearing a soft cotton base layer under compression can reduce direct friction.
- Inspect skin regularly. Check for redness, bruising, or irritation after each use, especially during the first week.
When to Avoid Deep Pressure Entirely
- Active skin wounds or healing surgical sites
- Areas with known vascular fragility (consult your specialist)
- During an acute subluxation or dislocation — pressure on an already unstable joint can worsen injury
- If you have vascular EDS, consult your medical team before using any form of deep pressure
Building a Safe Deep Pressure Routine With EDS
Start slow. EDS bodies respond differently to sensory input than neurotypical bodies do, and what feels good on day one may cause problems after extended use.
Week 1–2: Assessment Phase
Pick one compression garment — a compression shirt is usually the best starting point. Wear it for 30–60 minutes during a calm activity. Note how your body responds: Does proprioception feel clearer? Is pain better or worse? Any skin irritation?
Week 3–4: Expansion
If the initial garment is comfortable, add a second zone (compression socks, for example). Begin using a lightweight blanket (5–7% body weight) during rest. Continue monitoring joints and skin.
Ongoing: Personalized Protocol
Work with your OT or physiotherapist to develop a protocol that accounts for your specific EDS subtype, your most problematic joints, and your daily activity demands. Deep pressure for EDS isn’t one-size-fits-all. It needs clinical tailoring.
Frequently Asked Questions
Is deep pressure therapy safe for all types of EDS?
Deep pressure is generally safe for hypermobile EDS (hEDS) when using compression rather than heavy weight. Classical EDS requires careful material selection due to skin fragility. Vascular EDS requires direct medical supervision before any pressure application. Always consult your specialist before starting.
Can weighted blankets cause subluxations in EDS?
They can if the weight is too heavy or placed directly over hypermobile joints. Use a lighter weight than standard recommendations (5–7% body weight instead of 10%), keep the blanket below problem joints, and ensure you can always push it off independently. Compression blankets without added weight are a safer alternative.
Why do people with EDS crave tight clothing and pressure?
Poor proprioception from lax connective tissue means the brain receives unreliable position data from joints. Deep pressure provides clear, organized sensory input through skin-based mechanoreceptors, compensating for the proprioceptive deficit. The craving for pressure is the nervous system seeking the data it needs to feel grounded.
Should I see an OT for deep pressure with EDS?
Yes, ideally. An occupational therapist familiar with EDS can assess your specific proprioceptive needs, identify which joints to protect, recommend appropriate compression levels, and create a wearing schedule. Look for OTs who specialize in hypermobility or connective tissue disorders.
Do compression garments help with EDS-related POTS?
Medical-grade compression stockings (20–30 mmHg or higher) are a standard non-pharmaceutical treatment for POTS, which frequently co-occurs with EDS. They help by reducing blood pooling in the legs — and they simultaneously provide proprioceptive sensory input. It’s one of the clearest dual-benefit tools available for EDS management.

The DPS Editorial Team
Editorial Team
The DeepPressureStimulation.com Editorial Team researches and writes about deep pressure stimulation, weighted blankets, and sensory tools. We are not licensed occupational therapists or medical professionals. All content is based on peer-reviewed research, published clinical guidelines, and reputable health sources. Always consult a qualified healthcare provider before starting any new therapy.
Stay Informed, Stay Calm
Get science-backed articles on deep pressure therapy, weighted blankets, and sensory tools delivered to your inbox. No spam — just calm.
📬 No spam, ever. Unsubscribe anytime.